Lasers for Burn and Trauma Scar Rehabilitation
Written by Jill S. Waibel, MD on November 09, 2019
Dermatology has been at the forefront of laser invention and innovation in medicine. One such innovation has been the “fractionation” of laser beams. These fractional lasers have now become an impressive tool in treating burn scars. Laser treatment of scars represents a major innovation that heals in ways not previously possible.
A Breakthrough in Laser Science Leads to New Treatment
“Fractional” photothermolysis (laser resurfacing) has been the most remarkable breakthrough in clinical laser science since the development of “selective” photothermolysis, which enabled lasers to be used to treat targeted areas, while sparing the surrounding tissue. Fractional lasers create incredibly small, microscopic scars that the human body can heal quickly, allowing “remodeling” of the scarred skin layers to a more normal appearance. This method of skin resurfacing using a laser has led to clinical efficacy, or effectiveness, in aesthetic (cosmetic) procedures and scar treatment, with high physician and patient satisfaction.
This ability to remodel scarred skin via laser therapy is yielding results not previously possible. The human body can heal the smallest wound ever encountered (fractional wound) in scar tissue and the healing results in (almost) normal skin. In fact in 2013 JAMA Dermatology published a Consensus Statement entitled Laser Treatment of Traumatic Scars with an Emphasis on Ablative Fractional Laser Resurfacing, which concluded that scar treatment paradigms, or models, should include extensive integration of fractional resurfacing.
While reconstructive efforts can be limited by the development and persistence of pathologic scar formation, the best possible outcome for a patient who has experienced a significant injury can be achieved by coordinating the restoration of form and function. Both military and civilian research has revealed that fractional lasers can lead to both functional and cosmetic improvement. For example, patients often report improved range of motion with decreased pain and itching after one treatment. It also has been observed that scars continue to improve with each laser session. Given these results, the largest consumer market for lasers could potentially be in the treatment of scars.
How It Works: Fractional Laser Physics for Scars
Research over the last 10 years has improved our understanding of the clinical effects, histologic changes, molecular cascades, and minimal risks associated with fractional laser resurfacing.
Fractional laser technology was introduced into our “tool kit” as a unique concept to create a pattern of hundreds of microscopic thermal injuries to skin. Again, the purpose of creating this pattern is that it stimulates and allows the human body to create a more rapid healing, a type of healing and pattern of injury that allows for that “remodeling” of the scar tissue to a more normal appearance.
The mechanism of action for ablative fractional therapy is complex. With temperatures reaching more than 100°C (212°F), the treated areas of the epidermis and dermis are vaporized, or ablated. In essence, ablative fractional lasers create microscopic full-thickness wounds. Immediately after ablation, damaged epithelia is eliminated and the excessive build-up of collagen fibers in the scar tissue shrinks. (The thickness and amount of collagen present in scar tissue can affect the appearance of scars.) Over the next 3 to 6 months, new collagen, the fibrous structural protein found in connective tissue under the skin layer, forms. The series of wounds that are created lead to newly synthesized collagen and granulation tissue, then eventual regeneration of the epidermis. Repeated treatments have continued effects
with the greatest being on collagen formation—the new collagen forms in thinner bundles with this treatment, thus scar tissue shrinks and has a smoother appearance.
Lasers and Surgery: Synergy for the Treatment of Scars
The treatment of scars is a multispecialty endeavor. A combination approach by medical experts yields optimal scar improvements. If an injury heals in the presence of tension, hypertrophy often ensues. This condition is characterized by deposits of excessive amounts of collagen, as previously explained, giving rise to a raised scar. Understanding the role of tension in the development of a scar is essential to designing a successful treatment strategy. If there is significant hypertrophy or contracture present in a scar, surgical intervention is necessary to relieve the tension or there is a high likelihood the scar will reform. After tension relief, hypertrophic and contracture scars are more elastic with new remodeling of collagen and are more amenable to treatment with laser. However, if a scar has had initial fractional laser therapy this often makes surgical intervention easier to perform because the fractional laser therapy helps to create thinner collagen bundles.
Laser Therapy for Burn and Traumatic Scars
Erythematous scars (reddened scars caused by a dilation of superficial blood vessels in the skin, or erythema), and hypertrophic scars (scars with excessive deposits of collagen that cause a raised-scar appearance) are seen frequently in the first year after injury. Vascularspecific lasers and light devices, especially the 595-nm pulsed dye laser (PDL), are already well established for such applications. PDL is often combined with fractional laser therapy—either in the same treatment session or in alternating sessions.
Hypertrophic burn and traumatic scars are best improved by ablative fractional lasers. Ablative lasers, when compared to other lasers, have a significantly greater potential depth of thermal injury. One such laser modified for the treatment of scars reaches 4.0 mm in depth. Furthermore, tissue ablation appears to induce a modest immediate photomechanical release of tension in some restrictive scars. An appropriate degree of surrounding thermal coagulation appears to facilitate the subsequent remodeling response. To determine the appropriate laser pulse energy settings (treatment depth), scar pliability and thickness is estimated by the physician through palpation, or physical exam by touch.
Pigment-related abnormalities of scars (hypopigmentation, or a lack of coloring; hyperpigmentation, or darkening; and depigmentation, a loss of pigment) can also be improved with fractional therapy. Flat or atrophic scars from burns and trauma also respond well to fractional laser therapy. Atrophic scars are dermal depressions that occur due to collagen destruction during an injury. The goal of laser treatment for atrophic scars is to stimulate collagen production within the atrophic areas. Neocollagenosis, or collagen production, is most stimulated by fractional laser therapy, making it the best choice for flat or thin scars.
Fractional Laser Treatment: What to Expect
Any part of the body may potentially be treated with fractional laser therapy. The majority of fractional laser treatments can be performed in the clinic setting using a commercially available topical cream anesthetic preparation, which is applied under occlusion, or covered, 1 hour prior to treatment. Some patients may benefit from systemic preoperative analgesics (pain medication) or anxiolytics (anxiety medication). Conscious sedation or even general anesthesia can be employed in instances of large surface area involvement or anticipated poor patient tolerance of the procedure while awake. This is a particularly important consideration in children, as multiple treatments are usually required and children do not tolerate repeated painful interventions well. Patients experience minimal to no postoperative pain and little post-procedure downtime, resuming most normal activities after 48 hours.
With previous discussion in mind, fractional laser treatment technique, parameters, and adjunctive treatments should be applied thoughtfully to minimize the degree of cumulative thermal injury to the tissue. Each treatment is customized at every session according to individual scar characteristics and interval changes.
Lasers for Mature Scars
Fractional lasers are not only effective on new scars. Mature scars, whether 1 or 60 years old, all respond well to laser therapy. For the past decade we have treated scars of all ages. A minimum treatment interval of 2 to 3 months between fractional laser treatments is recommended to give the compromised scar tissue time to heal. Even after just 1 treatment session, a patient may continue to have improvement for many months up to 1 year.
Problems associated with mature scars include burning, itching, pain, discomfort, disfigurement, contracture, and limits to form and function. Fractional laser treatments have been successful not only in the appearance of scars but improving range of motion, while fractional ablative lasers also can have dramatic improvement in pain, itching, and burning.
I am currently honored to be in the process of treating Kim Phuc, who suffered the ravages of war as a 9- yearold child when she was burned with napalm during the Vietnam War. Her main complaint had been pain in her shoulder, where the fire bomb landed. Kim is now receiving laser treatments to reduce the damage to her body caused by the massive burns she suffered.
Lasers for New Scars – Intervene Early for Possible Prevention of Scars
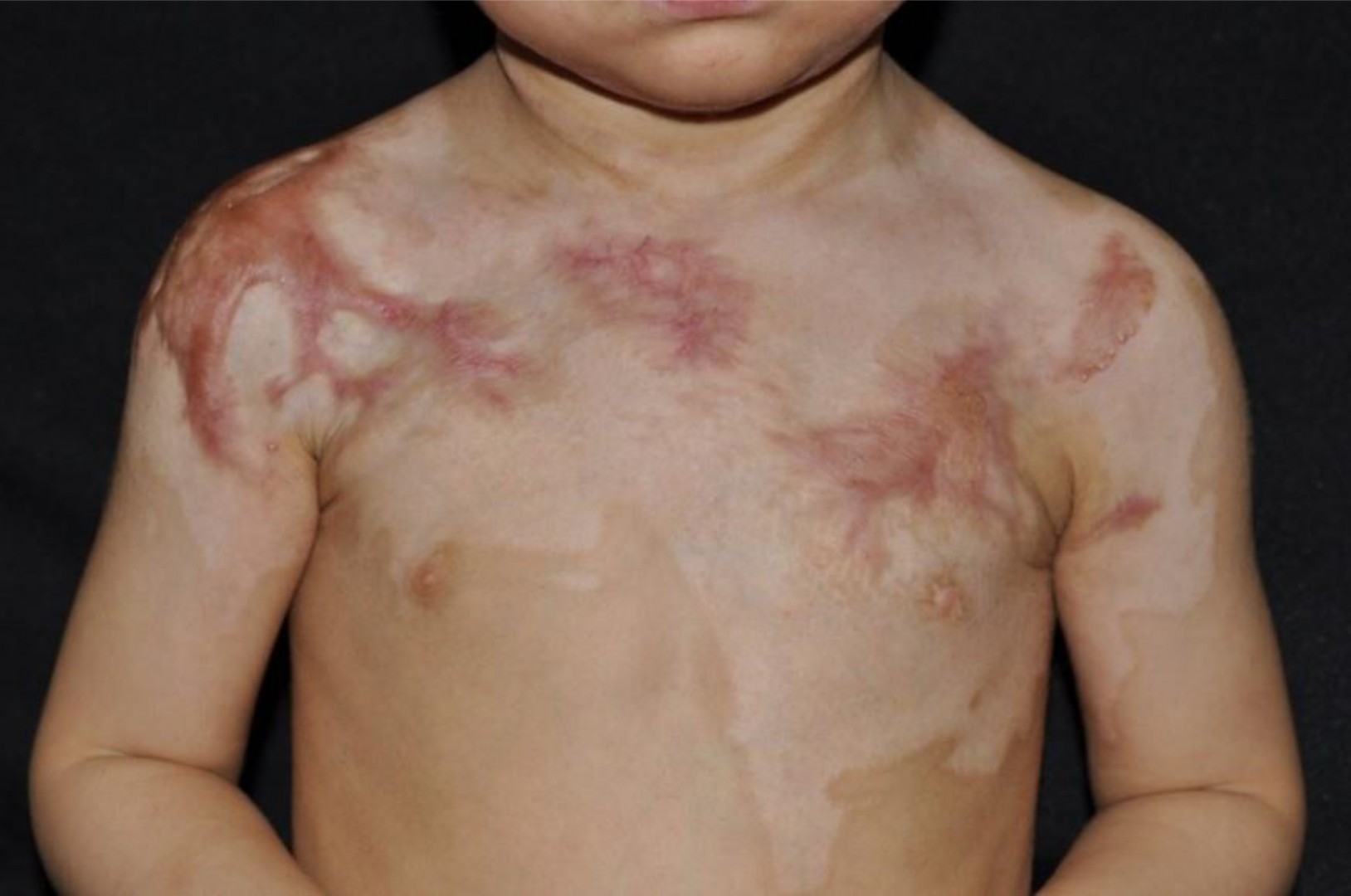

A 2-year-old child, 3 months post burn injury, before and after 2 treatments with pulsed dye laser, intense pulsed light laser, and fractional ablative laser.
Traditionally reconstructive efforts have been delayed until 1 year after injury, at which point many patients have formed hypertrophic scars and have significant decrease in range of motion. In fact, burn and traumatic scars worsen during the proliferation of wound healing between 3 and 7 months after injury. Early anecdotal evidence suggests that using fractional ablative laser in the early phases may improve wound healing and decrease hypertrophic scar formation. The discrete ablative columns likely have various wound-healing advantages, including novel laser photomicrodebridement, biofilm disruption, and stimulation of deep dermal cells. Fractional lasers in photo-aged (sun- or UV-damaged) and scarred skin have been shown to stimulate growth factor secretion, increase collagen production, and improve the cosmesis of skin, while producing negligible local trauma. This provides a unique opportunity in this patient population to improve short-term and long-term healing and has implications for all wound healing in medicine.
For the past 5 years in our office we have been treating patients with lasers after burn and trauma injuries within 3 months of injury. We have found that with early intervention fewer treatments are needed and that laser appears to have a powerful scar preventative effect. I am currently at the end of a 2-year clinical trial prospectively studying early intervention of fractional ablative CO2 laser with 830-nm LED phototherapy for acute burn injuries. Early laser intervention, especially in children, seems to melt away the scars, and fewer treatment sessions are needed.
Laser-Assisted Delivery of Drugs and Cells to Enhance Treatment
Laser-assisted delivery (LAD) is an evolving method using full-field ablative devices. Fractional ablative lasers first emerged in 2007 and provide a novel way to create a conduit, or “channel,” through multi-thick layers in the skin, including the stratum corneum, epidermal, and dermal layers, in a rapid, predictable, and controlled pattern. These channels serve as access points for drug delivery or cell delivery, such as stem cells or skin cellular transplant, and allow for more effective transport of actives deeper into the skin.
LAD with ablative fractional laser pretreatment has already been reported and evaluated in clinical studies for a variety of dermatologic conditions. LAD of such actives as triamcinolone acetonide, 5-fluorouracil, poly- L-lactic acid, bimatoprost, PRP, vitamin CEF, biofilm, epidermal skin transplant, and stem cells for scars has been studied.


Before and after LAD with fractional ablative laser and triamcinolone acetonide.
Working Toward Insurance Reimbursement for Laser Resurfacing
One major drawback to laser resurfacing of scars is that no medical code exists for insurance reimbursement. As we have researched this issue, it has become clear that one of our responsibilities as physicians is to advocate for our patients and to work with American Medical Association’s coding committee, Tricare (the provider of civilian health benefits for military personnel, retirees, and dependents), and Congress to get such codes in place. It takes time, effort, science and a lot of work to bring a code to existence.
To achieve that goal, a group of veterans, philanthropists, physicians, and politicians have formed a nonprofit foundation, Restoring Heroes, that will develop, implement, and integrate a regimen (a protocol of care and treatment) for burns and scar trauma within the Department of Defense and Veterans Administration healthcare systems for wounded, ill, and injured active duty and retired service members and their families, and veterans. The foundation will also work with Tricare, Congress, and the AMA/RUC (Specialty Society Relative Value Scale Update Committee) to establish additional codes to use laser and other cutting-edge modalities in the treatment of burn and trauma patients.
Summary
Since their introduction, fractional lasers have helped many adults and children who have scar deformities. Patients and their families are grateful for these medical devices. Personally it is very rewarding to be a physician who is part of improving a scar, regardless of whether the patient is an infant or an adult. The medical success of fractional lasers has added greatly to our ability as physicians to help heal our burn and trauma patients.
Dr. Jill Waibel is a board-certified dermatologist in private practice at Miami Dermatology and Laser Institute in Miami, Florida. She is also the subsection chief of dermatology at Baptist Hospital in Miami and a voluntary assistant professor of dermatology at the University of Miami’s Miller School of Medicine.